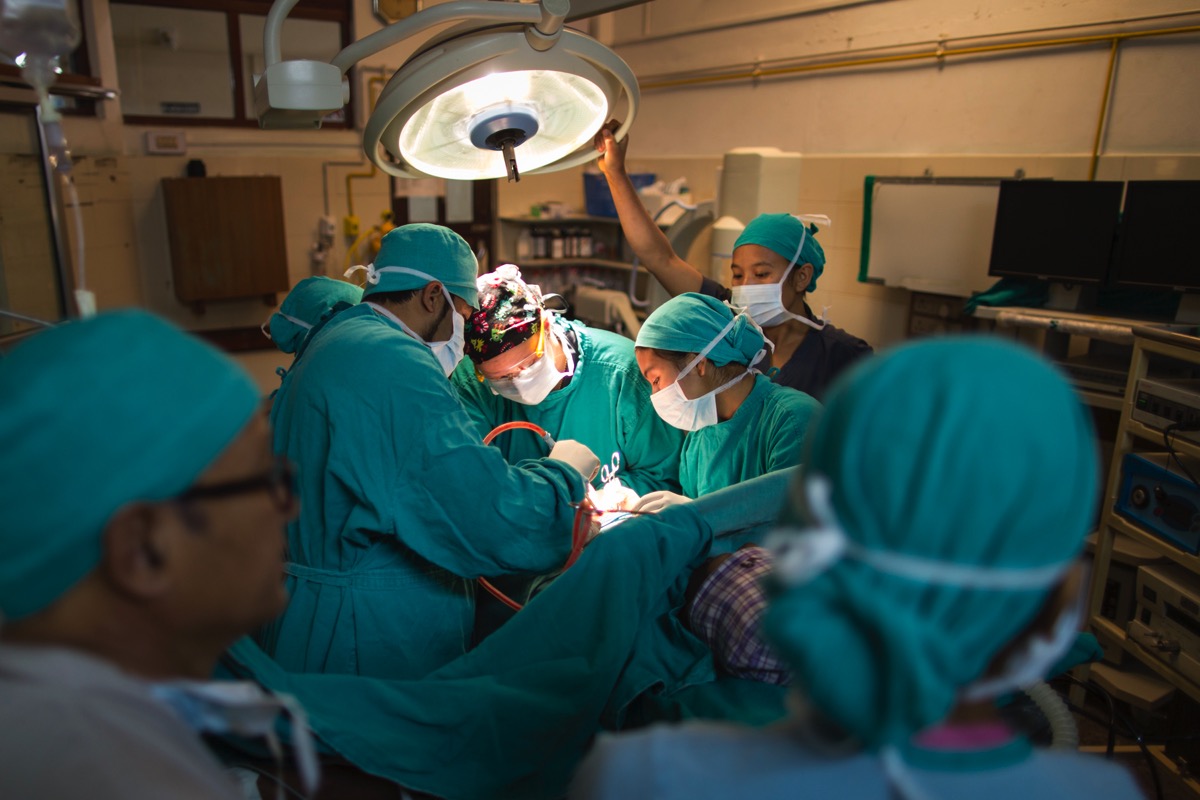
Last week I was the only senior surgeon in Tansen, as my colleagues were both busy. There is no doubt that Tansen needs more than one surgeon, so it was a busy week. Busy can be measured on more than one parameter, though. We can book less cases, which we did. We can have other surgeons cover the on call (here we have orthopaedic surgeons who share after hours call with us). We can’t really affect the emergency cases that arrive, though.
Some weeks just feel more busy because of the sort of cases that show up. A week with a couple of difficult emergency laparotomies will always feel more busy than a week with twenty paediatric hernias. A laparotomy is when a surgeon opens the abdomen of someone who is very sick and deals with what is inside, whatever it is. It is the operation that we do for perforated ulcers, perforated appendices, trauma and almost any other situation when a sick patient arrives with abdominal pain.
Laparotomies are more tiring than hernias because you have to make up the solution to the problem. Sometimes there is an accepted protocol of what is “best”, particularly for common pathologies, like perforated ulcers. But sometimes you have to use your training and experience to decide on an appropriate solution. Usually, there is no correct answer. Some solutions are more risky, but are great if everything heals well. If things don’t heal well, you get to reoperate – two operations for the price of one! Other solutions are ultraconservative. Different surgeons make their own decision about what to do, and then have to accept their choice. If the patient recovers well, or poorly, you re-examine what you chose – should you be more aggressive, or did you contribute to the decline. For all these reasons, big operations are more taxing than smaller – they simply come with more emotional and physical impact.
So the week was a tiring one because we had some serious cases to worry about. Luckily the evening case load was not too bad, and I have some good junior colleagues to work with me. But I missed having other surgeons around more than I expected.
Anyone who has worked with me will tell you I am a confident (cocky) surgeon. I know what I want to do, and I am happy to accept the outcomes of my decisions. I’m pretty happy to disagree with people if I think they are being stupid. I certainly don’t need people around to validate what I think. But I underestimated how much I like to work with smart people who have different opinions. When the evidence is not clear (welcome to surgery) and yet a decision has to be made, it’s really nice to combine the experiences of two or three people to make a decision. When you’re choosing to do something weird or unusual, its nice to have someone else say its a reasonable sort of crazy. Its nice to confess your mistakes to someone who has made similar mistakes in the past. We all know it’s terrible to have a bowel anastomosis leak, but surgeons also remember what it’s like to deal with it.
I didn’t feel stressed because I had to work every day, although days off are great. But I did miss the chance to discuss things with someone else, and to get a second opinion. This simple interaction is a keystone of most medical practice and is part of the reason confidentiality is tricky – we routinely discuss patients with other doctors. It’s a way to access the hive mind and I think it is probably more necessary in surgery, where formal evidence is poor. There is no absolute right way to sew two things together, and every choice has to be made taking lots of different things, including experience, into account.
I started to think about all the solo practitioners in the world. In Australia, remote doctors are pretty uncommon. However, in Nepal we have 2 trained surgeons per 100,000 population, well short of the recommended 30 (from lancet commission on global surgery). There are scores of hospitals and health posts run by a single GP or trained health worker. That person is responsible for looking after the medical, surgical and obstetric needs of their population, often with less years of training than our urban practitioners. We know that the world population should have access to three major surgical treatments – treatment of an open fracture, a caesarian section and a laparotomy. However, I often don’t consider the fact that those procedures are performed by someone who also treats high blood pressure, does the vaccinations and without access to many “core” therapeutic tools (like pathology, and sometimes X-ray). They refer elective surgeries to bigger centres, but when their dying patients arrive, they have to deal with all that emergency surgery entails – the decision to operate, the decision not to operate, and what repair to do.
I would like to salute all those solo health workers and GPs across the world. I don’t normally consider the difficulty of simply working alone, and it’s tough. You solo doctors (and health workers) serve a huge segment of the population. I imagine you get a lot of more trained, more supported doctors telling you you did it wrong. Let us remember that they are saving the rest of the world, the remote bit, without computers and internet – the bit that we don’t live in.
Some wonderful insights Cris. I take my hat off to all health professionals serving in the developing world. Thanks so much for sharing your life and giftings among the people of Nepal.